My Experience with Mental Health
During my first year of optometry school, I had a difficult transition that eventually led to challenges academically. I wish I could tell a straightforward story of how I didn’t know how to properly study or balance my academic life, and that working harder led to my success–but my story, as with any person’s story, is much more nuanced than that. Living with mental illness, my story often gets reduced by the common discourse around mental health that is shaped by the medical model of mental health and disability. The medical model defines a person by their impairments or differences, and focuses on how to fix or change these differences by medical or other treatments, with the goal of eventually curing a person so they can be normalized and reintegrated into society. Even language around mental health often uses stigmatizing words such as “suffering from” or “struggling with” a certain mental illness, and that the individual must be responsible for fixing what is wrong with them in order to be productive, functioning, and successful. Alternatively, there is the social model of mental health and disability. The social model focuses on the way society is organized and what barriers and opportunities are available for a person. It is not about what is wrong with a person, but rather what can be changed about the system or environment a person is in. Suddenly I realized that my difficult transition into optometry school wasn’t because of my mental illness–it was because accessing resources and support systems for me to thrive with my mental illness were particularly challenging in respect to my unique circumstances and marginalization of my identities. With this understanding of the social model of mental health, I became determined to share my experiences and work with others to shift the mental health discourse within my own community.
Mental Health During 2020
Fast forward two years to today, conversation about the increase in mental illness during the COVID-19 pandemic has become widespread. In a September 2020 article from Science,40% of surveyed graduate students in STEM had reported symptoms of anxiety and depression, increasing nearly 20 percentage points from 2019. When considering our optometric student community, I can only imagine how this has been a particularly difficult year,especially for our first year students or any students experiencing a drastic transition. But let’s remember to be specific about what’s causing this current increase in mental illness. This year’s COVID-19 pandemic and protests for racial justice brought us a heightened understanding of inequity and injustice–so when we speak about how COVID-19 has increased mental illness, we must speak specifically about the social and economic conditions that impact mental illness because doing so enables us to find tangible ways to shift our focus from awareness to action.
Student Action
Last year, a small group of us students formed a Wellness Committee to augment the existing mental health resources at our school and highlight events throughout the city that address mental health and well being. But this year, we recognized awareness and self-care
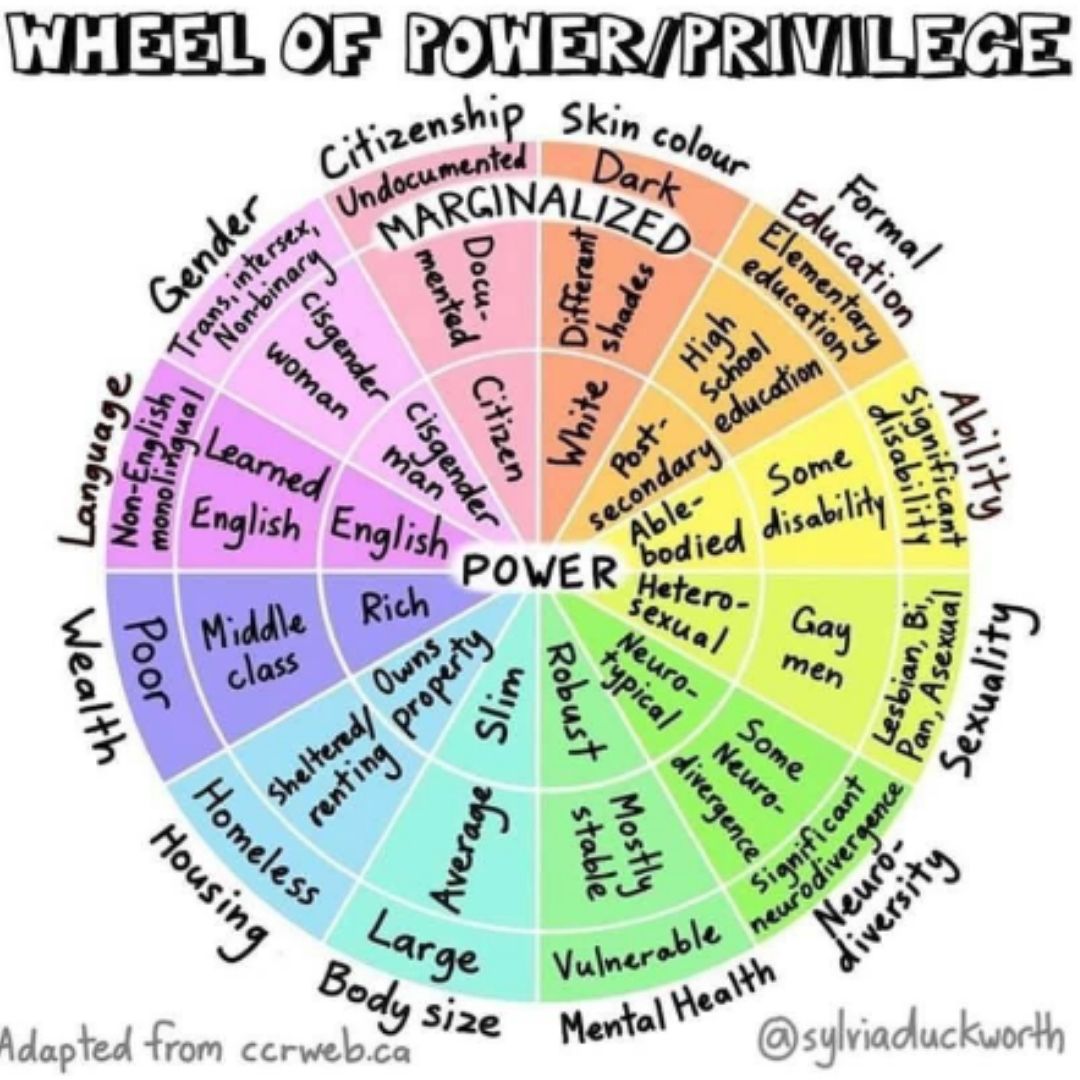
wasn’t enough. As diversity and inclusion efforts at colleges of optometry have been working to address systemic racism and the environments of our schools, we saw that ableism and mental health were often addressed separately or left out of this picture. Shining a light on privilege causes us to no longer assume that everyone can access the same routes of healing or have universally successful experiences with mainstream mental health care. We decided to form the first optometry school chapter of the national organization Project LETS (Let’s Erase the Stigma); a peer-led grassroots organization that centers the voices of people with lived-experience of trauma, mental illness, chronic illness, disability, and neurodivergence. Our goal became that of building: community care, peer support collectives, inter-sectional education,and our capacity for responding to and transforming harm.
What is community care?
Community care is how we will be able to begin addressing issues of oppression such as racism, xenophobia, Anti-semitism, Islamophobia, homophobia, transphobia, ableism, and soon. It is the ways in which we facilitate community interactions, conversations, and structures of support. It is rooted in how we hold empathy within groups and between groups, such as that of students, faculty, staff, and patients. It is our understanding that there are factors affecting all of us that self-care and individual pursuits of healing alone cannot achieve. When it comes to trauma and oppression of marginalized peoples and identities, we need relational healing.
What are different barriers to mental health support?

We cannot assume everyone has supportive friends and family, are able to talk to someone, has access to therapy or medication, has insurance, is able to advocate for themselves, is able to safely share their story, can access certain mental health language or information, or is empowered by the same resources. For example, not all students can feel safe sharing their experiences to individuals of greater hierarchical power such as faculty or administrators. Not all people find hotlines or textlines helpful during times of crisis, and could potentially be further harmed if police or emergency responders are called while in crisis. Our widespread discourse can also be a barrier to mental health support. As a community, challenging the medical model of mental health and disability, and opening up to other models could be a helpful tool for some to contextualize and navigate healing in a way that won’t further their feelings of being isolated and pathologized due to their experience. In doing so, we also can shift away from thinking happiness means being free or cured of mental illness. We can begin to view healing as a non-linear journey that is about the process more than it is about the end goal. Considering the intersections of a person’s identities, we must also recognize the barriers that exist due to systemic and societal marginalization and oppression. These are factors we don’t always consider when we are thinking about a student’s academic success.
What can peer support in optometry school look like?
Having structures for peer support is important because it breaks down some of the barriers listed above for accessing mental health resources. Peers can share their similar experiences and help their peers find autonomy and hope. For us, forming a chapter of Project LETS enables students with lived experience to apply to become Peer Mental Health Advocates (PMHAs) and be provided training by the national organization. This is a 16-hour training that isdeveloped by peers with lived experience, and informed by Intentional Peer Support (IPS) and Certified Peer Recovery Specialist (CPRS) curricula. PMHAs engage with a variety of topics during training including: principles of Disability Justice, the history of psychiatry,empathetic listening skills, crisis response skills, cultural competency in peer support,building crisis and safety plans, etc. Our hope in the future is to have faculty and staff become PMHAs for each other as well.
Why is community care important for the broader optometric community?
When we talk about community care, we are extending our responsibility of addressing mental health, ableism, marginalization, and harm to the greater community and society rather than the individual. With community care, we are viewing mental health through a disability justice lens. Our goal in optometry is to help people see, but through a disability justice lens, our goal is to prevent or reduce the impacts of visual disability and make environments more accessible. For example, it could even be as simple as ensuring a person with myopia has eyeglasses so they can learn at school–but through the social model of disability we know that accessing eyeglasses isn’t so simple for everyone. It is through these frameworks that a parallel between mental health and optometry exists, and we become better able to address the barriers for people with mental illness, and the barriers for our optometric patient community. Without recognizing this, the ableism that we internalize as students later becomes the ableism we practice with as optometrists.